Steroid Depletion: The Hidden Driver of Anxiety, Fatigue, and Hormonal Chaos — and the Complete Guide to Rebuilding
My biology was fragile from the start. Childhood wasn’t exactly a foundation of health - it was the opposite. My family moved constantly, which meant no stable rhythm. We spent years in the far north, where it was cold all the time and food was limited. I was sick often, and every infection meant another round of antibiotics. Looking back, my digestion, my bile flow, my whole system never had a fair shot at stability.
That weak foundation showed up everywhere later in life. Hormones breaking down, cycles and energy unstable, symptoms I didn’t even realize were connected. And when I went to doctors they never bothered to piece it together. No one mentioned that gut, thyroid, and hormones live in the same system or that when one goes down, the rest will follow.
So I started figuring it out myself. I read, experimented, tracked, rebuilt, and learned how steroidogenesis actually works. I learned that what looks like “normal aging” or “random bad luck” is really a predictable breakdown of the cascade that builds your hormones.
And here’s what I can tell you after years of trial and error: If you understand the map, if you nourish your biology the right way, you can have stronger steroidogenesis in your 40s than you ever did in your 20s.
What Steroid Depletion Feels Like
For women, it can feel like a monthly war. PMS becomes brutal, bleeding heavy or unpredictable, cycles either too short or vanishing altogether. Libido disappears, skin breaks out like you’re a teenager again, hair starts thinning, and sleep fractures into pieces. And what do doctors offer? Birth control or antidepressants, while progesterone - the hormone that could actually stabilize you - never gets a mention.
For men, the signs are just as clear. Morning erections fade, testosterone quietly slides downward year after year. You push harder in the gym but can’t build muscle, your drive collapses, belly fat accumulates. And instead of answers, you’re told to “try harder” or get on TRT, with no mention of the upstream block that started it all.
And for both men and women, the day-to-day toll is brutal. Cortisol dominates. You’re wired at night, dead tired in the morning. Recovery from anything - even a light workout - feels like a hangover. Mood flattens; some days you’re irritable, some days anxious, most days just empty.
This isn’t “normal aging.” It’s what happens when the steroid cascade collapses - when the raw materials and signals your body needs to build hormones have been shut down.
The Steroid Cascade
Every steroid hormone in your body - progesterone, testosterone, estrogen, cortisol, aldosterone - comes from one starting point: cholesterol.
That’s the first truth medicine buried. Cholesterol isn’t a villain - it’s the raw material of life. Without it, your body can’t build the hormones that keep you fertile, strong, and resilient.
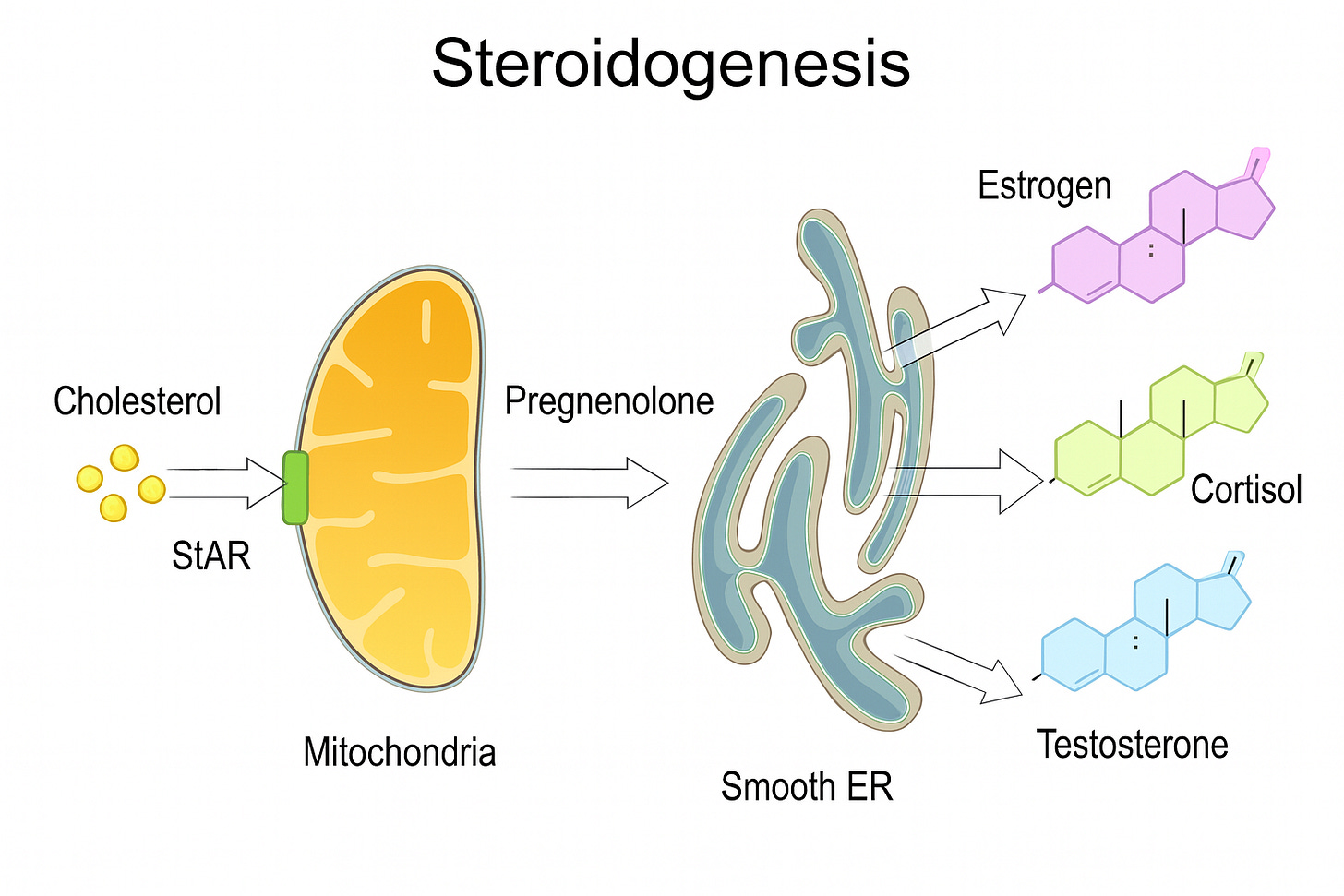
Step One: Moving Cholesterol Into Action
Cholesterol by itself is just sitting in your cells. To make hormones, it has to move into the mitochondria - your cell’s power station. The gatekeeper here is a protein called STAR (Steroidogenic Acute Regulatory protein). If StAR isn’t working, cholesterol never crosses the mitochondrial threshold, and steroid production collapses.
Thyroid hormone supports this step. T3 helps increase StAR expression and steroid output in tissues like the testes and adrenals. This is why low-thyroid states often come with “high cholesterol” blood tests but low hormone symptoms - the raw material is there, but it’s not being moved into action.
Step Two: Pregnenolone — The Mother Hormone
Once cholesterol enters the mitochondria, it’s converted into pregnenolone by the enzyme CYP11A1. This is the master branching point. Pregnenolone can flow in several directions:
Into progesterone (which itself is a precursor to cortisol and aldosterone).
Into DHEA (the precursor for both testosterone and estrogen).
Into cortisol directly, depending on which enzymes are active.
Pregnenolone is often called the “mother hormone” - not poetic, but accurate. If pregnenolone levels are low, everything downstream suffers.
In aging: Research shows pregnenolone and DHEA decline sharply by the 30s and 40s, independent of thyroid. This is one reason people describe feeling “older” long before labs look abnormal.
In stress: The “pregnenolone steal” is the concept that chronic stress diverts pregnenolone toward cortisol instead of sex hormones. Strictly speaking, it’s not theft - it’s enzyme preference. Stress enzymes like 17α-hydroxylase and 21-hydroxylase get upregulated, pushing pregnenolone and progesterone into cortisol. The result is the same: less progesterone, less testosterone, more cortisol dominance.
Step Three: The Branches
From pregnenolone, the cascade splits into the hormones you feel:
Progesterone: Calms the brain, protects bones, stabilizes cycles, balances estrogen. Also the intermediate for cortisol and aldosterone.
DHEA: Converts into both testosterone and estrogen, supports memory, immune resilience, mood and energy.
Cortisol: Essential in bursts (waking up, fighting infection) but destructive when chronically high. Diverts pregnenolone away from sex hormones.
Aldosterone: Regulates salt and blood pressure; when it’s low, people get dizzy on standing, crave salt, and feel weak.
Testosterone: Drives muscle, strength, libido, motivation, red blood cell production. Low in both men and women = flat drive, poor recovery, low confidence.
Estrogen: Needed in balance. Too much relative to progesterone causes PMS, breast tenderness, fibroids, and in men, fat gain + feminization.
Step Four: The Enzyme Gatekeepers
Each step requires enzymes - proteins that cut and shape the molecules. And each enzyme requires cofactors: vitamins and minerals. Without these, the whole chain stalls.
Vitamin A (retinol): regulates steroidogenic enzymes and STAR. Without retinol, ovulation and testosterone both falter.
Zinc: required for the enzyme 17β-hydroxysteroid dehydrogenase, which activates testosterone and estradiol. Low zinc = low testosterone and ovulation problems.
Magnesium + B6: regulate enzymes that calm cortisol and support progesterone synthesis.
Vitamin C: concentrated in adrenal glands; needed to make pregnenolone.
Selenium: protects thyroid and steroid glands from autoimmunity and oxidative stress.
Step Five: Stress, Inflammation, and Receptors
Here’s the part almost nobody talks about: even if your body makes hormones, they’re useless if your cells can’t hear them.
This is where stress and inflammation sabotage the system. They don’t just drain pregnenolone into cortisol; they scramble receptor function - the docking stations that let hormones deliver their message. Think of it as static in the communication line. The hormone is “there” on paper, but your cells don’t respond.
Endotoxin (LPS) and the gut–hormone axis
When gut bacteria die off (especially gram-negative species), they release endotoxin (LPS). A healthy gut and fast transit clears it, but with dysbiosis, slow digestion, or leaky gut, LPS spills into the bloodstream.
LPS binds to immune receptors (like TLR4), triggering an inflammatory cascade - IL-6, TNF-α, IL-1β. These cytokines directly suppress steroidogenic enzymes in the ovaries, testes, and adrenals.
Research shows LPS lowers testosterone production in Leydig cells, suppresses progesterone in luteal cells, and increases conversion to stress steroids instead.
It doesn’t stop there: LPS also interferes with thyroid conversion (T4 → T3), compounding the problem upstream.
Chronic inflammation and hormone breakdown
Inflammation accelerates enzymes like 11β-HSD that deactivate cortisol into cortisone, and others that destabilize androgen levels. The result: hormone swings and crashes instead of steady resilience.
Inflammatory cytokines can also increase aromatase activity - the enzyme that turns testosterone into estrogen. That’s why men under chronic stress and inflammation often show low T and rising estrogen.
In women, inflammation increases prostaglandins and worsens PMS, cramps, and heavy bleeding - symptoms of low progesterone effectiveness.
Receptor sensitivity — the silent failure
Hormone levels don’t matter if receptors won’t respond. Chronic IL-6 and TNF-α exposure reduce androgen receptor expression and blunt progesterone signaling. That means your labs can look “normal,” but functionally you’re still depleted.
Aging adds another layer: fewer receptors and less binding affinity. Studies show that by midlife, even with mid-range hormone levels, signaling is weaker. That’s why “normal” labs in a 45-year-old don’t feel the same as in a 25-year-old.
Stress chemistry rewires the cascade
Cortisol dominance suppresses GnRH and LH/FSH signaling - the brain’s instructions for ovaries and testes. That’s why stress alone can shut down cycles in women or collapse testosterone in men.
High adrenaline and cortisol also deplete cofactors like magnesium, zinc, and vitamin C — the very nutrients steroid enzymes depend on.
Over time, stress doesn’t just tilt the cascade - it rewires it. You become a body wired for survival chemistry, not fertility or vitality.
The Real-Life Translation
Hormone collapse isn’t just about making less. It’s about a body flooded with noise: gut toxins, immune cytokines, chronic stress signals, and aging receptor loss. That’s why people say, “But my labs are fine - why do I feel broken?”
Because production is only half the story. Signaling is the other half. And stress plus inflammation are what sever the line.
· You can have perfect cholesterol and still be infertile or anxious if thyroid isn’t activating STAR.
· You can have normal testosterone on paper but still feel weak and unmotivated if inflammation is blocking receptor signaling.
· You can have plenty of pregnenolone made but under stress it all flows into cortisol, leaving you sleepless, anxious, and sexless.
The cascade is not just a chart. It’s a living system.
It takes raw material (cholesterol), ignition (thyroid), clean pathways (enzymes + cofactors), and a calm environment (low inflammation, low stress signaling). If any of those break, your hormones collapse - not randomly, but predictably.
Why Modern Biology Breaks Here
If steroidogenesis is such a core human process, why are so many people hormonally wrecked today? Because almost every lever in the cascade has been systematically sabotaged by modern life.
1. The cholesterol war.
For decades, we were told cholesterol is the enemy. Statins, low-fat diets, plant sterols - all sold as “lifesaving.” What they actually did was strip away the raw material your body needs to make hormones. People with cholesterol under 160 mg/dL are routinely praised as “healthy” - yet those are the very people with infertility, low libido, fatigue, depression, and collapsed steroid output. Cholesterol is not optional; it is the foundation of your steroid economy.
2. The stress economy.
Modern life keeps us in cortisol-first biology. Work stress, sleep deprivation, stimulants, fasting, overtraining - all of it biases enzymes to funnel pregnenolone into cortisol at the expense of sex hormones. This is why so many women lose cycles under stress, and why so many men in their 30s have the testosterone of a man in his 60s.
3. Medications that mutilate the cascade.
Birth control pills flatten ovarian hormone rhythms and deplete B vitamins, zinc, and magnesium - the very cofactors steroid enzymes need.
SSRIs alter cortisol signaling and blunt sex hormone function.
Statins block cholesterol synthesis - removing the raw material at step one.
Finasteride (for hair loss) blocks 5α-reductase, crashing DHT and often libido permanently.
4. The gut-inflammation feedback loop.
Fortified foods (iron filings in your breakfast cereal), PUFA oils, antibiotics, and low-fiber processed diets create gut dysbiosis. That dysbiosis releases endotoxin, which suppresses steroidogenic enzymes and blunts receptor activity. This is why labs can look “normal” while you still feel hormonally flat. The receptor communication lines are jammed with noise.
5. Endocrine disruptors everywhere.
Plastics (BPA, phthalates), pesticides, flame retardants, heavy metals - all proven to mimic or block hormone receptors. They don’t just lower your levels; they scramble the signal so the body no longer responds the way it should.
6. The aging paradox.
Yes, DHEA and pregnenolone decline with age but modern biology accelerates this decline. Chronic inflammation, low thyroid, low cholesterol intake, and constant cortisol bias make people in their 30s feel like they’re 50.
And the cruelest part? Doctors call this “normal.” Women are told their PMS is just bad luck. Men are told low T is aging. Both are offered pills instead of repletion.
The Repletion Map for Steroids
If the cascade collapses in predictable ways, the good news is this: you can rebuild it in predictable ways too. The goal isn’t to hack one hormone at a time, but to restore the entire system so it flows.
Here’s the map.
Step 1: Restore the Raw Material (Cholesterol)
Your hormones are built from cholesterol. If you’ve cut eggs, dairy, red meat, or shellfish, you cut your steroid supply chain.
Eat enough animal foods! Eggs, dairy, liver, ruminant meat, shellfish. Very low-fat or plant-based diets flatten steroid output because they strip away cholesterol and saturated fats.
Ideal cholesterol for steroidogenesis is often above 160 mg/dL. Below that, steroid production is compromised no matter what your doctor says.
Practical tip: If your cholesterol is low, add two whole eggs a day, full-fat dairy, and ruminant fat (beef, lamb) - you’ll feel the cascade come back online faster than you expect.
Step 2: Ignite with Thyroid
Thyroid hormone (especially T3) drives StAR protein, the gatekeeper that moves cholesterol into mitochondria. Without thyroid, the assembly line never starts.
This is why hypothyroid people often have “perfect cholesterol” but still low hormones - the cholesterol isn’t being used.
Daily practice: Track waking temp and pulse. If your temp is consistently below ~36.6°C (97.8°F) or your pulse is under 70, the cascade is starved of ignition.
Eat frequent carbs + protein to refill liver glycogen and stabilize thyroid.
Light in the morning, low light at night to align circadian thyroid rhythms.
Consider cofactors like selenium and zinc to support thyroid conversion (see below).
Remember: steroids don’t build if your thyroid isn’t running or your liver is clogged. That’s why this article comes after thyroid and bile. Thyroid turns cholesterol into pregnenolone. The liver clears excess estrogen and keeps the balance.
Step 3: Nutrient Cofactors
Enzymes that convert pregnenolone into downstream hormones need micronutrients. Without these, the line stalls.
Vitamin A (retinol): required for progesterone, testosterone, and ovulation. Beta-carotene from plants doesn’t work. Get it from liver, dairy, eggs. Retinyl palmitate 2,500–5,000 IU/day if diet is low.
Vitamin E: protects sex hormones from oxidation, lowers PUFA damage. 100–200 IU/day mixed tocopherols (d-alpha + gamma) with meals that contain fat.
Zinc (with copper): from oysters, red meat, shellfish. Crucial for testosterone in men, progesterone balance in women. 10–25 mg zinc/day (gluconate, picolinate, or citrate). Always pair with 1–2 mg copper (liver, shellfish, or low-dose supplement).
Magnesium + B6 (P5P): calm cortisol surges, smooth cycles, stabilize mood, stabilizes ATP for steroid enzymes. Get it from fruits, root vegetables, dairy or supplement 200–500 mg/day (glycinate, malate, bicarbonate, avoid oxide). B6 (as P5P): 10–25 mg/day.
Vitamin C: highly concentrated in adrenals, needed to make pregnenolone. Get it from citrus, papaya, kiwi, potatoes.
Selenium: protects glands from oxidative stress and lowers thyroid/steroid autoimmunity. Get it from organ meats, seafood or supplement 100–200 mcg/day (selenomethionine).
B1 (thiamine/benfotiamine): enhances mitochondrial function and steroid enzyme efficiency. Thiamine HCl: 50–100 mg/day. Benfotiamine (fat-soluble, better cell uptake): 150–300 mg/day.
B2 + B12: support redox balance and energy metabolism for steroid conversion. Get it from dairy, liver, eggs.
Rule of thumb: You don’t need megadoses. You need steady intake from real food and strategic supplementation.
Step 4. Clear the Noise (Gut + Inflammation)
You can swallow all the cholesterol and cofactors in the world, but if the gut is leaking endotoxin and the liver is clogged, hormones won’t work.
Carrot salad or cooked mushrooms daily: bind endotoxin, lower estrogen burden.
Taurine, ox bile, betaine HCl if digestion is sluggish.
Salt with meals: supports aldosterone, blood pressure, and adrenal stability.
Avoid PUFA oils, fortified iron, and excess raw kale/lectins that irritate the gut lining.
Support gut lining with zinc, gelatin, glutamine, and saturated fats.
This is the piece almost everyone skips and why so many people “fail” thyroid or hormone replacement. Fix the gut, and receptors come back online. Read my article on Bile for more info on this.
Step 5. Manage Stress Chemistry (Pregnenolone → Cortisol Bias)
If your life is structured around cortisol, no supplement will save you.
Eat breakfast within an hour of waking to shut off the overnight cortisol surge.
Don’t train hard in a fasted state if you’re already depleted.
Use evening carbs (milk + honey, fruit + gelatin) to blunt night cortisol and prevent 3 AM wakeups.
Magnesium, taurine, and glycine can all dampen adrenaline and restore balance
Step 6: Advanced Supports (When Food and Basics Aren’t Enough)
For some, even with fuel, minerals, and digestion in place, the cascade still drags. This is especially true with age, where enzyme activity slows, receptor sensitivity drops, and stress leaves deeper marks. No matter how good your bile or thyroid are running, the body often needs targeted support to bring steroidogenesis fully back online.
But here’s the reality: dosing isn’t one-size-fits-all. The difference between a breakthrough and a crash often comes down to timing, context, and individual history. What follows are guidelines, not prescriptions - ranges that have been studied, used clinically, or proven safe in physiology. Always start low, move slow, and track your temps, pulse, and symptoms.
Progesterone (Progest-E): stabilizes cycles in women, calms the nervous system, and opposes excess estrogen. For me, it was the missing piece that finally calmed my system. The form I’ve used is Progest-E, a natural progesterone dissolved in vitamin E for high absorption. It was nothing short of lifesaving: it lowered my anxiety, let me sleep again, and gave me a sense of calm I hadn’t felt in years. It’s fat-soluble, so always take with food. Drops can be rubbed into the gums (sublingual/buccal) for faster absorption, or taken with a bit of fat if swallowing. For women in cycling years: best used in the luteal phase (after ovulation, roughly day 14–28) in doses of 3–10 mg/day at first, then adjusting as needed. In perimenopause or menopause, some use it more continuously in lower amounts but always titrate slowly. For men: only microdoses (1–3 mg) are sometimes used to balance excess estrogen or cortisol, never full female doses. Start small. With progesterone, more is not always better. Too much at once can feel sedating or flat. The goal is calm, stable, and restorative - not knocked out.
Pregnenolone: supports the “mother hormone” directly. Useful when stress has drained reserves. Typical support: 10–30 mg/day (oral or sublingual). Higher doses (50–100 mg) are sometimes used clinically, but many feel flat or overstimulated if they jump too high too fast.
DHEA (low-dose, cyclical): can boost energy and libido but must be balanced (too much = estrogen excess). DHEA declines steeply with age. It’s a flexible precursor that can convert to testosterone or estrogen as needed. But too much easily backfires with irritability, acne, or hair shedding. Typical support: 2–5 mg/day for women, 5–15 mg/day for men. Always start low and monitor carefully.
Testosterone therapy: Fix thyroid, cholesterol, and pregnenolone first. Often thought of as “the male hormone,” testosterone matters for both men and women - just in different amounts. It drives strength, motivation, libido, and tissue repair. When it falls, life gets flat. Sometimes DHEA alone is enough to restore androgen tone. In men with persistently low T despite fixing thyroid, diet, and stress: low-dose testosterone (gel, cream, or injections) can be considered but ideally in physiologic amounts, with careful tracking of free T, SHBG, estradiol, and hematocrit. In women, testosterone therapy is more delicate - microdoses only, usually as part of a broader hormone plan.
DHT and Androsterone (male androgen tone):
Testosterone isn’t the end of the line. Its strongest effects on libido, confidence, and muscle come from DHT (dihydrotestosterone). DHT is 2–5x more potent at the androgen receptor than testosterone itself. Modern stress, PUFA oils, inflammation, and meds like finasteride blunt DHT production. When testosterone therapy feels “flat,” low-dose DHT or androsterone can restore that missing edge. Typical support: 2–5 mg transdermal or oral. Androsterone is gentler than pure DHT, often giving a steadier, calmer androgen tone. Always stabilize thyroid, progesterone, and pregnenolone first, or DHT will feel like flooring the gas with no brakes.Estradiol (E2) This one is controversial. Many in alternative health circles oppose anything related to estrogen because they’ve seen the wreckage of estrogen dominance - the bloating, migraines, heavy bleeding, breast tenderness, mood swings. And it’s true: excess estrogen without progesterone is chaos. But here’s the other truth: if your estrogen is flatlined, that’s not health either. Women need estradiol for bones, brain, skin, vaginal tissue, and the proper signaling of the entire reproductive axis. Without it, collagen collapses, memory dulls, and vitality fades.
And here’s where it gets tricky: sometimes estrogen looks low on paper but is still high in tissues. That happens when clearance is blocked - the liver isn’t moving estrogen out through bile, the gut is reabsorbing it, or inflammation has made receptors hypersensitive. Labs can say “low” while symptoms scream “estrogen dominance.”
That’s why you never treat a number in isolation. Flat serum estrogen doesn’t always mean deficiency - it can mean estrogen is pooling in fat tissue, breast tissue, or even inside cells. First step is always restoring clearance: bile flow, thyroid support, liver cofactors (magnesium, B vitamins, glycine), and gut hygiene. Only once those channels are open does true deficiency or balance reveal itself.
If you’re still menstruating but your estrogen is genuinely inadequate: low-dose estradiol can be used only before ovulation, to support the follicular phase when estrogen should naturally rise. Always balanced by progesterone once ovulation occurs.
If you’re menopausal or fully without cycles: continuous low-dose estradiol is sometimes necessary, but it must always be paired with progesterone for safety and balance.
Typical support: 0.014–0.05 mg/day transdermal (patch or cream). These are small, steady, physiological doses - not the pharmacological “blast” often given in conventional HRT. The bottom line: estrogen is not the enemy. Out of balance, it wreaks havoc. In flatlined deficiency, it leaves the body brittle. In context, with progesterone, it can restore life.
Cynomel (T3): a direct thyroid support that raises temp and pulse quickly. Sometimes a tiny boost of direct T3 is what pushes thyroid fire into actual steroid building. Typical physiologic support doses are 2.5–5 mcg once or twice daily, always taken with food (carbs + salt) to prevent adrenaline surges. More is rarely better; it’s about nudging, not flooding.
Aspirin + vitamin K2: lowers inflammatory prostaglandins and frees up steroid pathways. A gentle support range is 81–325 mg/day, ideally divided, and always paired with vitamin K2 (100–200 mcg) to prevent clotting imbalance.
For more info on thyroid hormones, read my full breakdown in the dedicated thyroid article.
Why I Don’t Recommend Megadoses
If you dig around forums or anti-aging groups, you’ll see people throwing around huge doses of pregnenolone, DHEA, progesterone or androsterone. 50–100 mg pregnenolone. 25–50 mg DHEA for women, 100 mg for men. 20+ mg androsterone daily etc. On paper, it looks impressive: labs move, numbers go up.
Reality: flooding your system with precursors doesn’t guarantee balance. It guarantees chaos if the foundations aren’t set. Here’s what happens:
· Pregnenolone (50–100 mg+): Instead of flowing into progesterone or DHEA, stressed enzymes just shove it into cortisol. You get flat, spacey, or wired.
· DHEA (25–100 mg+): Converts aggressively into estrogen (in women) or both estrogen + DHT (in men). That means acne, hair shedding, irritability, or water retention.
· Androsterone (10–25 mg+): Pushes too hard on the androgenic lever. Yes, strength might rise for a while, but so can hair loss, irritability, and prostate burden in men.
My approach is different. I use physiologic support - doses close to what the body would naturally produce when nourished. Because here’s the truth: hormones are not gas pedals. They’re signals. If the thyroid, liver, bile, and minerals aren’t aligned, megadoses only amplify dysfunction. But if the foundation is restored, tiny physiologic doses feel like magic because the body finally knows what to do with them.
Labs That Actually Help
Here’s the problem: most doctors either don’t test hormones at all, or they run the wrong panels and send you home with “normal” results. But normal is useless if you feel broken. You don’t want average; you want optimal. And you want labs that match what your body is telling you.
Let’s break down what actually matters.
For Women
Progesterone: Test in the mid-luteal phase (about 5–7 days after ovulation). If it’s scraping the bottom of “normal,” expect PMS, anxiety, poor sleep, and cycles that come too soon. Progesterone is what steadies the nervous system and balances estrogen. Without it, you’re biologically in fight-or-flight every month.
Estradiol (E2): Should rise around ovulation, bringing energy, mood, and libido. But if estradiol spikes without enough progesterone to counter it, you get the classic estrogen-dominant storm: bloating, migraines, breast tenderness, and mood swings.
Ratio over raw numbers: A normal estrogen with low progesterone is still a problem. Always look at the balance - progesterone:estradiol. Optimal: At least 100:1 (when both are expressed in the same units, ng/mL for P and pg/mL for E2). Example: Progesterone 15 ng/mL, Estradiol 150 pg/mL → ratio = 100:1 (balanced). If progesterone is 5 ng/mL and estradiol is 200 pg/mL → ratio = 25:1 (estrogen dominant, symptomatic). When estrogen dominates, symptoms explode even if “the numbers” are technically in range.
For Men
Total + Free Testosterone: Total tells you how much you’re making. Free tells you how much is usable. Low free T with “normal” total almost always means high SHBG (sex hormone binding globulin) - often driven by stress, liver dysfunction, or excess estrogen.
Prolactin: Hugely overlooked. High prolactin kills libido, flattens mood, and erases morning erections. Doctors rarely check it, but it’s one of the fastest ways to explain “why testosterone therapy didn’t work.”
SHBG: This protein binds up testosterone and locks it away. High SHBG = low free testosterone, even if total looks fine. Stress, thyroid imbalance, and liver inflammation can all drive it higher.
Advanced markers (optional but powerful):
· DHT (dihydrotestosterone): If testosterone looks fine but energy, libido, or erections are still weak, check DHT. Low = poor androgen activation. Too high = hair loss, prostate issues.
· Androsterone (urine, via DUTCH test): Not in routine labs, but useful in stubborn cases. Shows how you’re metabolizing androgens. Low = weak androgen signaling; high = often linked with irritability, overstimulation.
For Both
Cortisol (AM + PM): Should peak in the morning to wake you, then drop through the day. If it’s flat, you’ll feel exhausted. If it’s reversed (low in the morning, high at night), you’ll get insomnia, anxiety, and that “wired but tired” feeling at 11 PM.
DHEA-S: Baseline of adrenal reserve. Low DHEA-S means your adrenals have been overworked - your “gas tank” is running on fumes.
Cholesterol panel: If total cholesterol is below 160 mg/dL, your doctor may call it “excellent,” but in reality it’s a red flag. Cholesterol that low = no raw material for hormones. That’s not heart health, that’s steroid starvation.
Nutrients that set the stage:
Vitamin D: modulates sex hormones and immune balance.
Magnesium (RBC test, not serum): cofactor for nearly every steroid enzyme.
Ferritin: tells you if iron is available for thyroid and ovarian/testicular function (too low = exhaustion, too high = inflammation).
B12: crucial for methylation and energy production. Low = fatigue and poor hormone synthesis.
The Rule That Matters
Always read labs in the context of symptoms, temps, and pulse. A “normal” hormone test doesn’t mean you’re fine if your body is still screaming depletion. Labs are tools - but your lived biology is the truth.
How to Get These Labs Without a Doctor
Most doctors won’t run the labs that actually matter or they’ll only run them halfway and tell you “everything is fine.” That doesn’t mean you’re stuck.
You can order many of these tests directly through private lab services online (search “direct-to-consumer labs” in your country). They partner with LabCorp, Quest, or regional labs, and you pay out of pocket. No insurance battles, no gatekeeping.
Blood draws (standard hormones, nutrients, thyroid): Can be done through private lab networks for ~$30–$150 per test. Panels for sex hormones, thyroid, and nutrients are widely available.
At-home hormone tracking (urine/strips): There are now home kits that measure LH, progesterone, and estrogen metabolites with urine strips or readers. They’re useful for cycle mapping if you’re a woman, or for confirming ovulation without relying on symptoms alone. They don’t give the full story, but they’re a useful layer of data.
DUTCH test (urine hormones + metabolites): This is the deep dive - it maps cortisol rhythms, estrogen/progesterone/testosterone breakdown pathways, and how you’re actually metabolizing them. It’s not cheap, and it’s more advanced than most people need at the beginning. I’ll be doing a separate article just on DUTCH because it deserves its own breakdown.
Rule of thumb: Start with bloodwork + symptom tracking (temps, pulse, sleep, cycles, libido). Layer in home testing strips if you want daily cycle data. Reach for DUTCH only once you’ve covered the basics, because it can overwhelm without context.
Signs You’re Rebuilding Steroids
This is where it gets good. When the steroid cascade finally comes back online, the changes aren’t subtle - they’re unmistakable.
For me, the first thing I noticed was sleep. After years of 3 AM wakeups with my heart pounding, I slept through the night and woke rested. That alone felt like a miracle. The anxiety that used to sit on my chest every morning started dissolving. Soon after, the warmth came back - my hands and feet stopped being ice blocks. And then the drive returned, the kind of inner push that doesn’t come from caffeine or willpower, but from biology actually working.
For women, it often shows up in the cycles first. Bleeding becomes predictable instead of chaotic. PMS softens. Progesterone calms the nervous system so you’re not white-knuckling through the luteal phase every month. Sleep improves, anxiety fades, libido and natural lubrication return. Skin clears, hair stops shedding, bones even feel sturdier. It’s the body remembering its rhythm.
For men, the first sign is primal: morning erections. They come back, and they’re reliable. Testosterone starts driving strength and motivation again. Training feels like progress instead of punishment. Muscle builds, belly fat recedes, mood steadies. The apathy that made everything feel gray gives way to an assertive energy - the kind that makes you want to move, compete, and claim life again.
And in both men and women, the transformation runs deeper than just numbers. Sleep becomes restorative - you don’t just “rest,” you rebuild. Stress doesn’t crack you in half anymore; you bend but don’t break. Energy steadies into something alive, not wired or jittery. Skin literally changes - it looks brighter, fuller, alive in a way that makeup or creams can’t fake. People start asking what’s different. And perhaps the most important shift of all: you wake with purpose again. There’s a current of vitality pushing you forward that was absent for years.